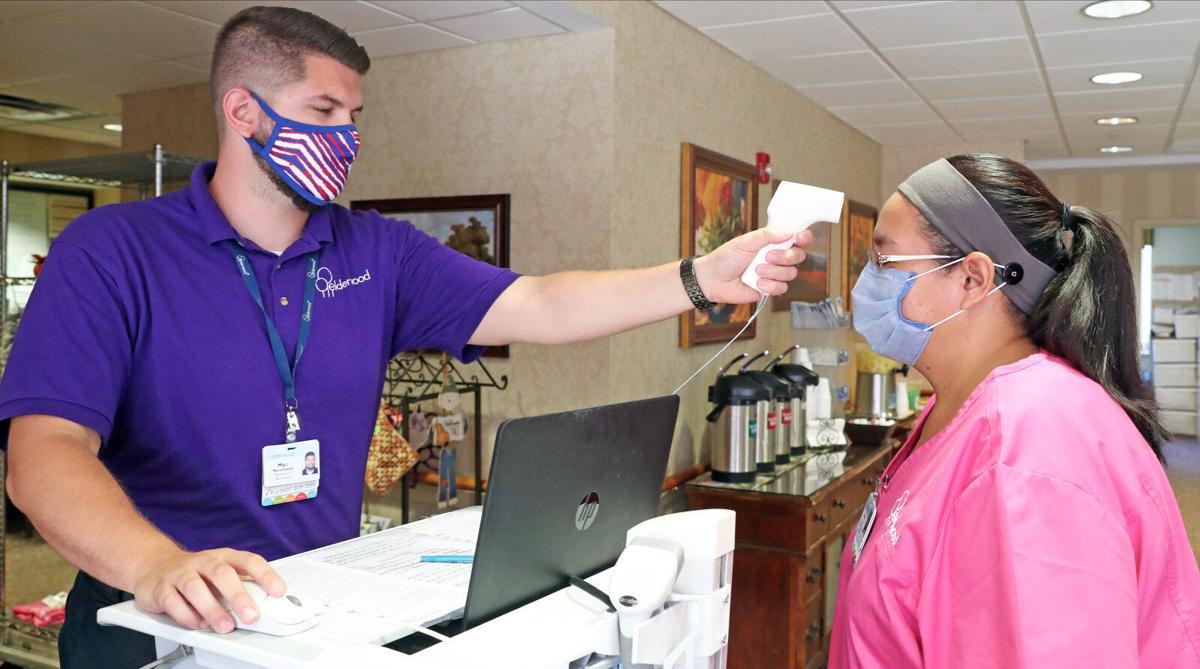
If a second wave of coronavirus arrives, what will be different? Third story in a series.
The first wave of coronavirus took a terrible toll as it swept through nursing homes in the spring.
Eighteen facilities in Western New York reported at least five Covid-19 deaths among their residents before July 1. Eight of those exceeded 20 deaths.
But as a second wave looms, nursing home administrators say they are in a good position to avoid that kind of death toll again.
What makes them so confident?
They point to their progress over the past couple of months.
People are also reading…
And they cite all the testing that is now being done.
Erie County has had 279 confirmed deaths from Covid-19 in nursing homes through Saturday, but only 20 since July 1, according to the state Health Department.
The state says Niagara County hasn't had a single Covid-19 death inside a nursing home since June, leaving its total at 44.
Schoellkopf Health Facility in Niagara Falls is another example of improvement. Eight patients died of Covid-19 there – but none since early June, according to the state.
From then through Sept. 13, federal testing statistics show, only one more Schoellkopf resident contracted Covid-19, even though 20 Schoellkopf workers have tested positive for the virus since mid-May.
"The testing has been very important in enabling us, if somebody is positive, to isolate them, or if it’s a staff member, to remove them from the schedule," said John Durno, the administrator at Schoellkopf. "We’re in on it a lot quicker if there’s any outbreaks or any positives."
From Niagara Falls to Rochester, the region is bracing ahead of a feared uptick in cases as early as September or October.
Besides testing, other measures to quell the pandemic in nursing homes included a ban on visitors, which is now being relaxed, and Gov. Andrew M. Cuomo's reversal of the order that required nursing homes to admit Covid-positive patients being released from hospitals.
“All those things contributed to stopping cold the ability of Covid to come into a facility," said Daniel J. Stapleton, the Niagara County public health director.
'Manage the disease better'
Those in the industry generally agree regular testing of employees for the virus was the key change.
"You control the environment as best you can. That’s probably one of the best ways you can do that," said Mark A. Sullivan, CEO of Catholic Health.
On May 10, Cuomo ordered all nursing home employees to take a Covid-19 test twice a week. That was cut back to once a week on June 10, but the results have enabled operators to do a better job of keeping staff who might have been infected outside the facility from spreading it to the elderly residents.
Cuomo senior adviser Rich Azzopardi said Thursday that "the main source of infection in nursing homes was, through no fault of their own, asymptomatic staffers."
“The measures that we take to protect the residents are much greater than they ever were when we first started to learn about this," said Pat O'Connor, vice president for long-term care operations at Catholic Health. "My sense in the community is that other facilities, too, have learned how to manage the disease better. The weekly testing of the staff is one of the most important things that we’re doing to catch any kind of virus early and keep it from spreading.”
Bill Hammond, senior fellow for health policy at the Empire Center for Public Policy, an Albany think tank, isn't so sure the Cuomo order is responsible for the lower number of deaths.
“It’s really hard to know for absolute certain," Hammond said. "Just the fact that the state issues an order doesn’t lead automatically to a decline."
Added Hammond: "Nursing homes are cut off from the world to some extent, especially when you cut down visitors, but still, the staff live in the community. If the virus is in the community, it’s going to get to them.”
Nursing home officials say what happens outside the walls of nursing homes can be a big factor in the health of those living inside.
“I can’t predict whether there’s going to be a second wave. I can tell you, based on numbers, that communities’ infection rates certainly will impact what is seen in nursing homes," said Rebecca Littler, chief nursing officer for the Elderwood nursing home group.
"If community spread and the infection rates increase, the risk of individuals who live in the community and then work in our homes, the risk of an individual coming in with the virus and then being an asymptomatic carrier is a huge concern for every nursing home," Littler said. "Until we have point-of-care testing daily before an employee comes in the door, they’re never going to stop 100% of the transmission risk.”
Read the full story about understaffing in nursing homes from News Staff Reporter Lou Michel.
'Learned as we went along'
Federal statistics don't agree with the state's data in detail. The U.S. Centers for Medicare and Medicaid Services, unlike the state, tries to track the deaths of residents after they are transferred to hospitals or other facilities from nursing homes.
CMS does list a few more local deaths since it started gathering weekly data in mid-May.
CMS also reports weekly numbers of positive Covid-19 tests among residents and staff. In almost every local facility, those numbers for residents have shrunk to single digits, or even zero, for weeks at a time.
As of Sept. 1, New York hospital or nursing home patients who may have died of Covid-19 must undergo a post-mortem test within 48 hours of death, unless next of kin refuses, and the Health Department's earlier statistics are being revisited.
“One thing we can agree with our legislative colleagues on is that accurate and reliable data should drive smart public health decisions," state Department of Health spokesman Gary Holmes. "So not only are we carefully reviewing all previous data, as the commissioner committed to, but we're also requiring confirmatory and post-mortem testing for anybody who may have had Covid-19 or flu symptoms, or exposure to someone who did, to ensure data integrity."
Even with the questions about statistical accuracy, it's apparent nursing homes are coping better than they were five or six months ago, and that the progress can be built upon to respond to the next wave, if or when it comes.
"While we all fear a second wave of Covid-19 as we enter the flu season, preparedness is a saving grace the second time around," said Jeff Jacomowitz, spokesman for the Buffalo Center and Ellicott Centers for Rehabiliation and Nursing.
Those two Buffalo facilities totaled 26 patient deaths early in the pandemic, Jacomowitz said, but both are now Covid-free. Federal statistics show no new cases at either site in recent weeks.
"Both facilities have learned since the early days of this pandemic that this is not a 'one size fits all' scenario and both Buffalo and Ellicott Center, like all nursing homes, learned as we went along what we needed to do to keep everyone safe," Jacomowitz said.
O'Connor of Catholic Health said research was not available in March on the length of time people with the virus remain contagious. She said that would have changed Catholic Health's procedures on when infected staff could return to work.
“We found out later that they may still have been shedding the virus," O'Connor said. "As soon as we did learn the research that was out there, we changed that process and policy ourselves.”
The return of some visitors
Such trial-and-error methods have produced improvements in managing the pandemic, which local health care leaders said should prevent things from getting worse in nursing homes – even if the situation worsens in the outside world.
But there are concerns that a more liberal visitation policy, which began Thursday, might put some of that progress at risk.
Visitation resumed last week at nursing homes and assisted living centers across New York, although mingling comes with tight requirements.
Visitors may enter, masked and socially distanced from loved ones, if they have written proof that they have had a negative Covid-19 test in the previous week.
“It’s smart to make sure those folks are tested the way the staff is," O'Connor said.
“I do believe that it is a necessary protection," said Littler of Elderwood. "We obviously don’t want families to come into the building if there is active transmission occurring and take it home to their families, so there’s protection on both sides. The visitation guidelines that are out are sufficient and needed."
From March 13 to July 15, the state barred nursing homes from accepting any visitors at all, leading to stories about families gathering outside an exterior window and shouting to their loved one inside.
That was later changed to allow visitors to facilities that had 28 consecutive days without a positive Covid-19 test for a resident or employee. That threshold was later reduced to 14 days.
“It’s really hard to criticize a policy for being too restrictive after how bad things got. We weren’t restrictive enough, so if the state overcorrected a bit, I feel that’s understandable," said Hammond of the Empire Center.
“We’re happy to see the rates have stayed lower, but we don’t know what’s around the corner," Durno said. "Hopefully with everybody’s awareness of the virus and more sanitary procedures, washing your hands, wearing masks, etc., it should alleviate any further issues.”