Gunfire is so common in her Buffalo neighborhood that Theresa Cox has thought about packing a pistol when she tends her garden and flowerbeds.
She'd love to get help fixing the backyard fence that young people battered last summer, while running for cover when gunshots broke out during a barbecue on the next block.
Most of all, she wishes the city would replant trees in the medians on Woodlawn Avenue. She misses the majestic look of the block where she used student loan money 43 years ago to buy a house where she and her husband, Donald, raised their four children.
“It’s a big world and we’ve been left out of a lot of it,” Cox said from her front porch this week.
The 69-year-old retired machinist, who worked 38 years in the aerospace industry, has always lived within a mile or so from the site where an 18-year-old, self-avowed racist is accused of using a modified assault rifle last Saturday to kill 10 people – all Black – and wound three others at a Tops supermarket.
People are also reading…
It inflicted yet more trauma on a community, city and country where most citizens view gun violence as crime.
Those on the front lines see something else.
A public health tragedy.
“We have a crisis in racism, a crisis in gun violence, but also a crisis in the lack of services, including a lack of access to mental health care,” said Dr. Joseph Sellers, who grew up in Buffalo and is president of the Medical Society of the State of New York.

Dante Oden, left, and Marcus Barnes outreach workers with two gun-violence prevention programs in Buffalo, chat Wednesday with Theresa Cox, who since 1979 has lived in the neighborhood that was the site last weekend of a racially motivated mass shooting.
Garen J. Wintemute, an emergency medicine physician at UC Davis Medical Center, is widely viewed as the first health care professional to 35 years ago reframe gun violence as a health issue, a construct barely recognized before the last decade, as the number of mass shootings intensified in the United States.
It took on greater proportions this year, after the New England Journal of Medicine shared research in April that gun-related fatalities during each of the last five years surpassed motor vehicle crashes as the leading cause of injury-related death for American children and those up to age 24, and the Centers for Disease Control and Prevention reported earlier this month that the U.S. homicide rate climbed 35% in 2020.
The mass shooting in Buffalo last weekend provided yet another example why many in the health field – frustrated that gun safety debates all too often start and end with talk of more background checks and renewed automatic weapons bans – look to reframe the gun-violence conversation as one focused on finding a broader array of data-driven solutions.
“It may be that the solutions here are 1,000 small steps,” said Sellers, who works in Cooperstown as a health system administrator and has three grandchildren who attend school in the neighborhood where Cox lives.
The statistics
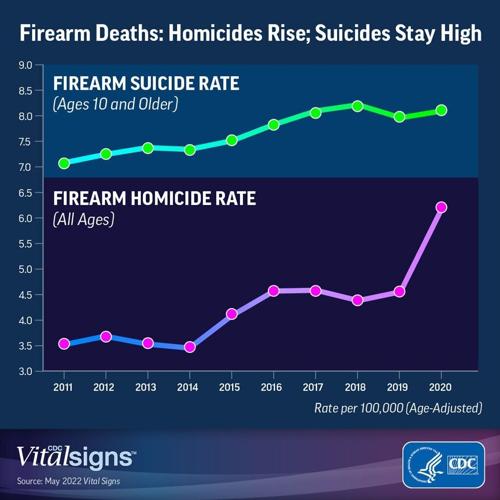
The CDC reported a record 45,222 gun deaths 2020, the latest year for which complete data is available.

Homicides accounted for 19,384 of those deaths – nearly 5,000 more than the previous year.
Suicides accounted for 24,292.
Another 611 fatalities involved legal intervention, 535 were accidental and 400 were from undetermined causes.
The Johns Hopkins University Center for Gun Violence Solutions further examined the numbers to find that the overall gun death rate among children and teens under 19 increased by 30% from 2019, driven by a 40% jump in the gun homicide rate and 11% increase in the gun-related suicides.
“Most folks don't know that most gun deaths are suicide,” said Cassandra Crifasi, deputy director of the center and an associate professor in the Johns Hopkins Bloomberg School of Public Health who specializes in gun violence research and prevention.
Those injured by guns each year is roughly double the amount of those killed, said Patricia Logan-Greene, an associate professor at the University at Buffalo School of Social Work who specializes in a trauma-informed approach to violence and childhood adversity.
“They may have lifelong disabilities, but people rarely look at that,” she said. “Then of course, every individual who was killed or injured exists within a family and a community. And every individual around them is also affected when you have a massive community trauma. The public health impacts go way beyond just the sheer the number of mortalities we have from firearms each year. It really reverberates, especially in the communities that are hardest hit by this.”
“The thing that really pulls together all of these shootings – whether they're homicide, unintentional, domestic violence-related, mass shootings, whatever they may be – is the firearm,” Crifasi said. “Between 80% and 90% of suicide attempts with a firearm resulted in a fatality. We know that in 2020, 80% of all homicides were committed with a firearm. People will say, ‘Guns don't kill people, people kill people.’ I say, ‘People with guns kill people, because it makes it much easier to cause harm to oneself or others.”

“We need to be focused on prevention,” says Cassandra Crifasi, associate professor in the Johns Hopkins Bloomberg School of Public Health who specializes in gun violence research and prevention.
Changing the process
“We’re overemphasizing the wrong kinds of things” with zero tolerance laws that lean on police, courts and prisons for every solution, Crifasi said.
The public health approach is that gun violence is everybody’s problem.
“When we see a shooting,” Crifasi said, “whether it's a terrible mass shooting like we saw in Buffalo, or a domestic violence incident, or a dispute that results in a shooting or a fatality in some of our cities across the country, public health folks tend to think immediately, ‘Where were missed opportunities to intervene? Was there a tool that wasn't used or a connection that wasn't made that could have prevented this? From the public health perspective, it is far more effective and inexpensive to keep something from happening in the first place than try to deal with the issue after the fact.”
Sellers said the addiction crisis underlined that you can’t stop overdoses by making drugs illegal but need a scientific approach to learn what works best, adjusting as evidence and results become more clear.
He and Crifasi agreed that putting a dent in gun deaths involves a greater emphasis on gun safety.
They support legislation that requires a waiting period and background checks prior to the purchase of all firearms, including person-to-person transfers, internet sales, and interstate transactions of all firearms.
They advocate greater use and coordination of extreme risk protection order laws, or “red flag” laws, which temporarily remove firearms when someone is deemed a threat to themselves or others. The medical society is committed to educating doctors about using that mechanism, which is available in 19 states, including New York, but rarely used and closely scrutinized when applied.
“It does us a disservice if we remove considerations around access, and availability of firearms, when we're talking about these shootings,” Crifasi said, “because it removes an option, a target of intervention, from the table.”
Other approaches include community-based violence intervention programs, more vigilance to stop social media radicalization of would-be killers, a greater emphasis on mental health, and wraparound services for victims and perpetrators of gun violence.
“We need to be focused on prevention,” Crifasi said.
Sellers believes a regional approach, like that used preserve the Great Lakes, would be a great first step to build more consensus nationwide.
A formal connection between the Center for Urban Studies and the Community Health Equity Research Institute at UB is sharpening the focus on Buffalo’s built environment and its impact on the city’s social determinants of health.
On the ground
Paula Kovanic-Spiro is program director of Buffalo Rising Against Violence at ECMC, or BRAVE, a violence intervention program launched in late 2019 at Erie County Medical Center, the Buffalo region's adult trauma center. It focuses on the structural causes of violence and provides survivors the tools and connections to make lifestyle changes that prevent re-victimization or further perpetration of violence.
Kovanic-Spiro, trained in public health and social work, came from Pittsburgh to start the program. She helped counsel the surviving victims and families in the 2018 Tree of Life Synagogue shootings in 2018.
She and her staff in Buffalo see poverty and other social determinants of health – including differences in education, employment, income, transportation, crime rates and the cost of child care – as drivers of gun violence.
Kovanic-Spiro also oversees SNUG Buffalo, short for Should Never Use Guns, which began more than a decade ago as an anti-violence ministry in the City of Good Neighbors to mediate conflicts and reduce shootings and homicides.
That effort caught the attention of the state Division of Criminal Justice Services and Office of Victim Services, which has resulted in BRAVE and SNUG working jointly since 2020 in an arrangement being duplicated across New York.

Gun-violence prevention outreach workers, including Dennis Brown, left, and Dante Oden, have been visiting residents every day on the streets surrounding the site where 10 were killed and three wounded May 14 at a Buffalo supermarket.
The SNUG office sits in the Bailey-Kensington neighborhood but its leaders, social workers and case managers – considered “credible messengers” – spend most of their time in sections where the latest crime data signals the greatest areas of need.
Several on staff have been crime victims themselves. They have spent every afternoon since the mass shooting in the neighborhoods surrounding the scene, to learn how they can help residents cope with their latest brush with gun trauma.
They consider ECMC their ground zero, making sure that no patient who has been a victim of violence leaves the hospital without a “warm handoff” for support that comes from SNUG workers and ECMC social workers, case managers, and a part-time psychologist.
Team members will ask about fears, needs and longings, and take tangible steps that can help make life more manageable and healthy over time. It might mean helping someone find a job or affordable housing, ensure consistent transportation or a healthy food supply, or move a potential shooting target out of the region.
Outreach case worker Tecrette Gist said she and others then will make regular contact going forward to help gun victims and their families build healthier lives.
Oishei Children’s Hospital – which has seen double the typical volume of gun-violence patients during the last two years – also works with the two programs.
“Gun violence impacts children of every race, children that live in urban, suburban and rural areas, and it happens every single day across this country,” said Dr. Stephen Turkovich, chief medical officer. “In almost all cases, children are killed accidentally or as bystanders of shootings that target adults.”
The aftermath often involves re-living recent and past traumas, Turkovich said, and fears of returning to a home or neighborhood where the violence took place.
Tears flowed this week, he said, while Oishei employees who live on the East Side shared accounts with colleagues about their children, fearful of going to school and having their parents and other loved ones leave the house.
“In my mind, the biggest problem addressing this trauma is a lack of unity, that as the country becomes more and more polarized, and everything becomes a partisan issue, we are moving further away from solutions," Turkovich said. “In my mind, mental health, homicide, suicide, racism, that's not partisan. These are human issues that we need to work on together.”
Such hard and painful work continues with greater determination in the Cold Spring neighborhood where Cox raised her family.
They know it won’t be easy, but Buffalo and other cities don’t close their hospitals because they can’t save everyone from cancer and heart disease.
Cox recalled this week how her kids complained growing up that Woodlawn Avenue was too quiet. Now she and her neighbors would like speed bumps on the side-street to lower the number of fast cars and fender-benders. She remembers how she and her husband, who died in 2017, used to walk down to Main Street and back after working second-shift jobs. She wouldn’t dream of doing that now.
“If you take a walk down your street, you're always looking over your shoulder,” she told SNUG workers on Wednesday. “You expect maybe a bullet would catch you. But I never expected a white kid to come into this neighborhood, drive (more than 200) miles. … I couldn't believe that. How do you kill people you don't even know? Had he taken the time to get to know somebody, he wouldn't have done it.”
Gist and other SNUG members listened intently as she talked, with hopes that more will listen, too, and help solve a life-shattering American crisis.
Understanding trauma
Trauma involves feeling scared, angry or shocked, wanting to hurt the person who hurt you, being embarrassed, feeling guilty and feeling numb.
Its common symptoms include feelings of hopelessness or helplessness and loss of control, mood swings, anxiety, depression, anger, nightmares or flashbacks, headaches or upset stomach, and conflict or withdrawing from friends and family.
Get support
Erie County Warmline: Free confidential non-crisis phone line, 716-248-2941, and text line 716-392-2221, for people having difficulty coping with life experiences. Open 4 to 11 p.m. daily.
Erie County Crisis 24-Hour Hotline: Counselors are available to talk with those in need at 716-834-3131.
211 WNY: Visit 211wny.org or call 211 anytime in the region for a free and confidential link to health and human services, including community resources for many health, social, mental health, substance use and developmental disability services.
The National Alliance for Mental Health Helpline: 716-226-6264, namibuffalony.org
Mental Health Advocates of WNY: Regional resource for mental health support, 716-886-1242, mhawny.org.
Suicide prevention: Anyone contemplating self-harm can call the 24-hour National Suicide Prevention Hotline at 800-273-8255.
email: sscanlon@buffnews.com
Twitter: @BNrefresh, @ScottBScanlon
In this Series
Complete coverage: 10 killed, 3 wounded in mass shooting at Buffalo supermarket
-
Updated
Hochul pledges pursuit of justice after shooting, calls on sites to crack down on white supremacist content
-
Updated
Sean Kirst: In Buffalo, hearing the song of a grieving child who 'could not weep anymore'
-
Updated
Recently retired police officer, mother of former fire commissioner both killed in Tops shooting
- 307 updates