Nobody's perfect, but in the health-care industry perfection is the standard - even a slight error can have dire consequences.
Tucson Medical Center health-care providers including Valesha Keith say they are feeling a lot better about reaching that perfect standard now that an improved electronic system is double-checking their work.
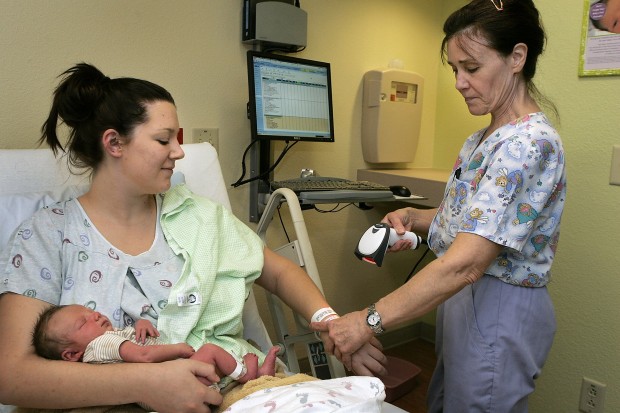
"It's a confidence boost," Keith said, after scanning the bracelet of a patient with a scanner similar to those used at grocery store checkouts, and then scanning a bar code on a packet of two pills. A computer attached to the scanner confirmed that the dosage and medication matched the prescription for Keith's patient.
The scanning process is now part of the protocol at TMC, which administers 220,000 medications every month.
Since a $30 million upgrade to its electronic medical records system launched June 1, each patient at TMC has received a bar code printed on a hospital bracelet. Before health-care providers do lab tests or administer any kind of medication, they must first "scan" the patient.
People are also reading…
In its first three months, the system sent out nearly 1,500 "wrong medication" alerts that providers subsequently corrected, hospital data show.
"Some medication names sound similar. Then others are sustained release or continuous release. The system always knows the difference," TMC pharmacy director Gilbert Romero said.
Electronic medical records are among requirements for hospitals under the new federal health-reform law. But when it comes to digitalizing medical systems, the term "electronic medical records" can mean many different things, said Frank Marini, a vice president and chief information officer at TMC.
"We implemented our electronic medical records in 2002, but until this year we still had paper patient charts," he said. "Paper is inefficient. The paper chart doesn't allow for timely, accurate, complete information. It has significant limitations."
The 642-bed nonprofit hospital began a process of upgrading its electronic system at the beginning of 2009 and spent the next 18 months working toward a completely paperless system.
TMC is one of just 145 non-government U.S. hospitals and the only one in Tucson that is at the near-top-level "stage six," according to an electronic medical records ranking system that goes from zero to seven. The ranking system was developed by HIMSS Analytics, a Chicago-based company that analyzes health-care data relating to information technology, costs and management metrics, health-care trends and purchasing decisions. The other Arizona hospital that has achieved state six, according to HIMSS, is the Casa Grande Regional Medical System.
In order to achieve stage 7, hospitals must be able to share with one another. That's not yet happening in Tucson, though a local nonprofit organization called the Southern Arizona Health Information Exchange is working towards that goal.
At the moment, if TMC needs patient information from another hospital, it must either request a fax of the information or send someone over to the other hospital to get copies of the records.
While businesses such as airlines and banks switched over to electronic records years ago, the health-care system has been slower to go paperless. While many doctors and medical experts tout the benefits of electronic records, the barriers to adopting them - time and money - are high.
About 30 percent of local doctors have converted to computerized medical records, according to Pima County Medical Society data.
UA Healthcare Inc., the local nonprofit entity that resulted from the merger of University Medical Center Corp. and University Physicians Healthcare this summer, is upgrading its electronic medical system, too. UA Healthcare includes two hospitals, University Medical Center and University Physicians Hospital at Kino.
While both hospitals have their own electronic medical records already, officials have prioritized getting UMC, UPH at Kino and their outpatient clinics on the same electronic system.
They also have plans to add the bar coding of patients and medication in the near future, said Shirley Gabriel, vice president and chief information officer for UA Healthcare.
The federal government's Veterans Affairs system of hospitals has been ahead of the curve for years. The VA system first went digital in the early 1990s and has been bar coding its patients and medications for nearly a decade, said Pepé Mendoza, a spokesman for the Southern Arizona VA Healthcare System.
Having that technology in place was "such a blessing when (Hurricane) Katrina hit," Mendoza said. "We received a lot of evacuees who were veterans and it made their care so much smoother to have them plugged into the system. We knew their health concerns right away.
"Electronic records just make it a lot easier to provide quality care."
Contact reporter Stephanie Innes at sinnes@azstarnet.com or 573-4134.