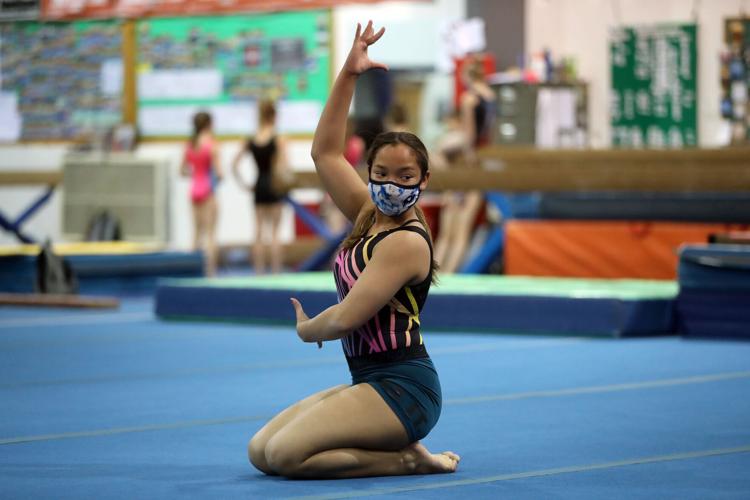The comedian Dan Soder stepped onstage at Helium Comedy Club in May, removed a protective spit screen from a microphone, and started making people laugh, poking fun at patrons, himself and, predictably, at the pandemic.
“We remember before the DISEASE!” Soder said.
We do, but even more importantly, what do we remember from this pandemic that will help us reclaim – or redefine – what’s normal? How can we go forward so that attending shows and sporting events and going to schools, offices and your best friend’s home all feel safe and routine?
Our weekly “Pandemic Lessons” series has probed questions about life with Covid-19 by tapping into the expertise of top doctors, scientists and other experts from across the United States and beyond. Here are the top lessons we learned in 2021:
People are also reading…
1. It’s up in the air
We have become amateur infectious disease specialists, figuring out whether a gathering is safe by answering self-imposed questions: Is everyone vaccinated? If not, did they have Covid-19 recently? Is anyone immunocompromised? How’s the ventilation?
We continued the habit of opening windows to keep air moving, and maybe even invested in a portable air cleaner with a HEPA (high-efficiency particulate air) filter. We listened to the advice of people like virologist Angela Rasmussen of the Vaccine and Infectious Disease Organization in Saskatchewan, who told us humidifiers “help by increasing your body's ability to defend itself,” and aerosol scientist Linsey Marr of Virginia Tech, who told us to set those devices between 40% and 60%, because that’s “the sweet spot” where the virus “decays quickly.”

“It’s like a friendly reminder of what things used to be like,” New York actor and comedian Dan Soder said of performing stand-up at Helium Comedy Club in May 2021.
2. Embrace small pleasures
Covid-19 life is coldest in the dark winter, unless you get outside and enjoy small pleasures: Crisp air. Hot chocolate. A perfectly packed snowball.
Yale University psychiatrist Dr. Paul Desan, an expert in seasonal affective disorder, told us 90% of people experience at least one change in “mood, energy, outgoing-ness, appetite, sleep (or) weight” during the darker, colder months.
His advice: Look to the Nordic countries, where winters are long.
“It’s part of the culture there to go outside early … and say, ‘Let’s go for a walk.’ ” Desan said, adding, “Exposure to light is just part of the culture … People understand that this is vital for their health.”
3. Worshiping is healthy
From an epidemiological standpoint, worship services evoke caution: packed groups of people reciting, singing, rejoicing – and breathing each other’s indoor air.
But engaging your spiritual side is one of the healthiest practices you can do. Dr. Harold Koenig of Duke University has conducted years of research showing that attending worship services is associated with lower risk of cancer, healthier blood pressure, longevity and better mental health. It is “the most powerful factor in terms of health benefits.”
But individuals and worship leaders should “follow the advice of public health officials,” said James Martin, a Jesuit priest and author of “Learning to Pray: A Guide for Everyone.”
“Bishops, pastors, ministers, rabbis, imams and others are trained in ecclesiology, not epidemiology,” he said. “The individual believer is also obliged to listen to public health officials, to ensure not only that they are able to keep healthy but, more importantly, that others are, too. It’s an exercise in charity towards others.”
4. Loneliness is an epidemic exacerbated by the pandemic
Loneliness and social isolation are associated with increased risk of heart disease, stroke, premature death and developing dementia, and increased rates of anxiety, depression and suicide. A 2015 study by researchers from Brigham Young University likened loneliness to the dangers of smoking 15 cigarettes a day.
Surgeon General Dr. Vivek Murthy has written a book on the issue, which he has likened to an epidemic, and here in Buffalo, retired Rep. John LaFalce has spoken out on it.
“Individuals can be imprisoned in themselves – in their loneliness,” said LaFalce, a longtime advocate for the elderly. “What we need to do is visit them out somehow: reaching out, caring, helping.”
He offered an idea: “Wouldn’t it be wonderful if just about every block in a village or a town had a block party?”

Sara Rockwitz, shown here at Gymnastics Unlimited in West Seneca, is one of 70,000 children in the United States who lost a parent to Covid-19. Sara's father Doug died on Dec. 23, 2020, the same day Sara came out of quarantine from her own bout with the virus.
5. Kids are not exempt
In the spring we met Sara Rockwitz, a 14-year-old gymnast training five days a week and trying to push her legs (“They just felt like jelly”) and lungs (“It was really hard for me to breathe”) back to competitive shape after a December bout with Covid-19.
While Sara’s experience followed a well-known pattern – 10 days quarantining in her bedroom; taste and smell disappearing for months – it wasn’t her family’s greatest struggle. She likely caught the virus from her father, Doug, whom she last saw 14 days before Christmas 2020, when she waved to him from the top of the stairs as he headed to the hospital.
He died 13 days later.
Sara is one of more than 167,000 children in the United States who have lost a caretaker to Covid-19, according to the “Hidden Pain” report released earlier this month by the Covid Collaborative.
“More than 70,000 children have been deprived of a parent,” the report says. “Nearly the same number have lost a grandparent who lived in the home. At the extreme of this need, more than 13,000 children have lost their only in-home caregiver.”
6. Travel is (mostly) safe.
Vaccinations increased, businesses reopened and the travel industry rebounded. But as Covid-19 persists and evolves, people can still get unnerved by travel. It’s not the act of traveling that puts you most at risk; airplane air is heavily filtered, and a KN-95 mask will protect you well in more crowded airport queues, as well as buses, trains and Ubers.
It’s what you do on your trip that can make you vulnerable. A popular example with Western New Yorkers is Florida, which in many spots is largely open and mask-free. That’s OK if you’re taking a walk along the coast.
“You’re outdoors, there’s usually a nice breeze at the beach, and there’s just really very low risk of transmission in that situation,” said Cindy Prins, an epidemiologist at the University of Florida.
Standing at a crowded bar, however, is not so smart. But in fairness to Florida, the presence of the virus looms large, and that’s a fluctuating factor over time. Over summer, most of Florida was deep red, while much of New York was a relatively safer yellow. That reversed this fall and early winter, meaning you’re mathematically more likely to run into Covid-19 in Erie County than in most parts of Florida.
Travel as you will, but be cautious everywhere – even near home.
7. Perceptions divide us
Masking vs. not. Vaccinated-only events. The factors that divide us have become more distinct during the pandemic, as has the connection between our political views and personal health decisions.
University at Buffalo researchers undertook a study funded by the National Science Foundation to analyze risk perception during the pandemic. They found that sociodemographics are influential. For example, people who are older, white, have school-age kids and lean Republican are more likely to believe in conspiracy theories about the pandemic and vaccination.
Communications Professor Janet Yang and her graduate student Jody Wong analyzed what people find scary (psychologists call this “dread risk) and mysterious (“unknown risk”). People who buy into conspiracy theories, they found, also perceive a higher dread and unknown risk toward vaccination.
“Misinformation seems to add to more uncertainties about the vaccines relative to the pandemic,” Wong said.
8. Immunity is a quest, not a status
Vaccines have lowered infections, intensity of illness and hospitalizations. But we learned vaccine-induced immunity wanes, and boosters are necessary. Post-infection immunity, meanwhile, is meaningful, too. But it is difficult to measure, and, in part, depends on how symptomatic you were. Generally speaking, more symptoms lead to higher immunity.
“You could get the sniffles or you could end up in the hospital on a respirator,” said Dr. Sumit Chanda, a San Diego-based infectious diseases expert at Scripps Research who is a Williamsville native. “Your immune response is going to be different.”
Now, enter Omicron, which typically presents milder infections, but is excellent at evading the first layer of immune defense. What we’ve learned is that Covid-19 immunity isn’t a status to be achieved; it’s an unending quest.
9. Disliking masks doesn’t mean they’re unnecessary
Masks aren’t fun. But for a virus that spreads in and out of our noses and mouths, good face coverings – such as surgical masks, at minimum, or preferably KN-95s or N-95s – do help.
For proof, look at hospitals, which have used them for years when patients have influenza, tuberculosis or other airborne infectious diseases.
“If you both stuff the virus if you’re infectious, and you block the virus if you’re trying not to get infected, it’s going to work, right?” said Dr. Thomas Russo, chief of infectious disease at the University at Buffalo’s Jacobs School of Medicine and Biomedical Sciences.
Researchers from Stanford and Yale recently published a peer-reviewed study that reinforced the effectiveness of surgical masks, which cut Covid-19 infections by 11% across the group of about 350,000 people. That’s with only “less than half of the population wearing masks,” said Dr. Ashley Styczynski, an infectious disease fellow at Stanford and one of the study co-authors.
That percentage may seem low, but for a virus that spreads exponentially, the ripple effect of eliminating one in 10 infections is much larger. “Even if you can't get everyone on board,” Styczynski said, “more masking is always a win.”

Ed and Katie Grzybowski watch as their son Lucas steps off the school bus after a day at kindergarten in November 2021. Lucas, a patient at Oishei Children's Hospital and Roswell Park Comprehensive Cancer Center, was diagnosed with a form of leukemia at age 5
10. It’s not nearly about you
As restaurants, schools and major events fully reopened, people who are immunocompromised started facing increased risk. Those of us around them have the ability to help.
Take Lucas Grzybowski, who learned in May 2020 – when was 5 – that he has a form of acute lymphoblastic leukemia. His cancer is treatable, but through an intense two-year regimen at Roswell Park Comprehensive Cancer Center that weakens his immune system and makes him more vulnerable to Covid-19.
“If your kid gets a fever of 102, they say, ‘OK, just give them some Tylenol and they’ll be all right,’ ” Edward Grzybowski said. “If my kid gets a fever of 100.4, you drop what you’re doing and get them straight to the hospital.”
The lesson we’re still learning: When you make health decisions, don’t just think of yourself, or your family. Think of people like Lucas.