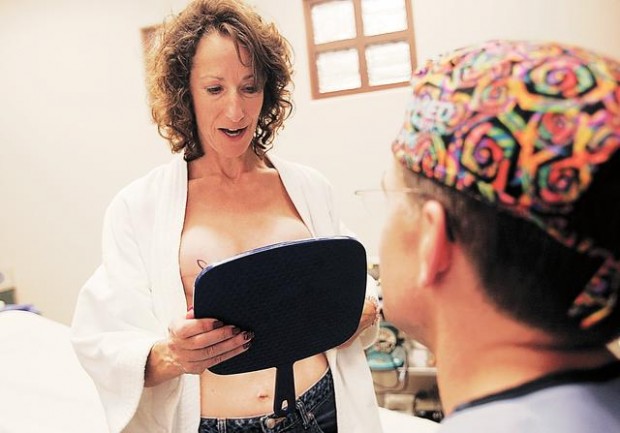
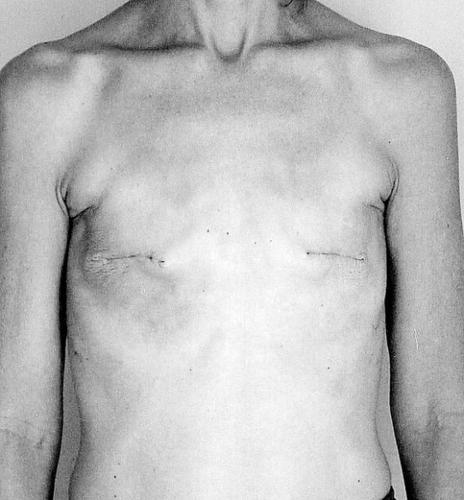
Mindy Diamond-Rivera had her breasts removed and she's ready to get rid of her ovaries and uterus. "Everything's coming out," said the 47-year-old patient of the High-Risk Breast and Ovarian Cancer Clinic at the Arizona Cancer Center.
Her mother, grandmother and great grandmother all died of breast cancer before the age of 43, and she's determined to use modern medicine to avoid the same fate.
"It's life, or death. That's it."
Diamond-Rivera's chance of developing breast cancer before her surgery was 87 percent — a number determined by genetic testing.
After her mastectomy, her risk of breast cancer is reduced by 90 percent. An oophorectomy — removal of the ovaries — reduces her risk of ovarian cancer by 96 percent. She talked with her doctors and chose removal of the ovaries and uterus — even though there's no firm evidence that her genetic mutation is linked to uterine cancer.
People are also reading…
Not every woman faced with this decision is as certain about it as Diamond-Rivera, but as geneticists identify more women with "the breast cancer gene," more women will be considering their options.
Among those women will be Diamond-Rivera's daughter.
Drastic solution
Diamond-Rivera worried for years that she would get breast cancer.
As a 12-year-old, she watched her mother die of breast cancer, and later she learned that the disease also took her grandmother and great-grandmother before they were 43.
"When is it going to hit?" Diamond-Rivera, 47, would repeatedly ask herself. "Every year when I celebrated my birthday I thought, 'OK. One more year. Is it going to skip me?' "
Over the years, she asked her regular gynecologists what she could do and always heard the same response: annual mammograms.
Then she found the High-Risk Breast and Ovarian Cancer Clinic, which sees patients two days each month. It opened at the Arizona Cancer Center more than a year ago.
In September, she learned from genetic testing that she carries the BRCA-1 genetic mutation, known as "the breast cancer gene." It is associated with an 87 percent chance of breast cancer and up to a 60 percent chance of ovarian cancer.
In November, she had her breasts removed, reducing her breast cancer risk by 90 percent.
Next month, doctors will take out her uterus and ovaries, reducing her risk for ovarian cancer by 96 percent.
Developing one of these cancers after the surgeries would be extremely rare, said breast surgeon Dr. Christina Kim, a founding member of the high-risk clinic.
"It feels like a weight has been lifted from my shoulders," said Diamond-Rivera, a former teacher who now instructs others how to teach in the Tucson Unified School District.
"I'm going to have a chance to see grandchildren. My mother never had that chance," she said.
Diamond-Rivera is one of about 200 women with a family history of breast and ovarian cancer who have come to the High-Risk Breast and Ovarian Cancer Clinic since it opened. There the staff tests patients for the BRCA-1 and BRCA-2 genetic mutations that are linked to these cancers, and advises high-risk women about their options, which range from monitoring their breast health to undergoing preventive surgery.
Only about 10 percent of all breast cancer cases are linked to these genetic mutations. Doctors aren't sure what causes the other 90 percent of cases, but research points to environmental factors, like obesity and a woman's estrogen exposure.
For Diamond-Rivera, in addition to the maternal link, her Ashkenazi Jewish heritage placed her in a group with higher rates of the genetic mutations for breast and ovarian cancer.
The clinic does not keep track of how many women have surgeries like Diamond-Rivera, but Kim says she performs them occasionally.
There are no national statistics about how many women have chosen this route, according to American Cancer Society representatives. Most women who choose surgery are past their childbearing years, but some are as young as 20 or 30 years old, Kim said.
Surgery was the clear choice for Diamond-Rivera, who knew she wanted her breasts removed even before she was certain she carried the genetic mutation.
Although some friends and family members thought she was acting hastily, the dread of being diagnosed with breast cancer had seeped into her daily existence. She talked about the threat of cancer with her family and children.
Those fears were borne out when doctors found precancerous cells in her breasts after they were removed.
Ironically, having her mastectomy was the easy part, physically and emotionally.
"It didn't really faze me like I thought it would," she said.
She was out shopping just a few days after the surgery and jokes that some of her friends didn't notice that she'd had the surgery.
"I'm thin, very thin, up top, and I was an A-cup bra size," she said.
Getting breast reconstruction was much more painful, but she knew she wanted it done.
"I still feel young, and I want to feel like a woman and have a sex life," she said.
To form her new breasts, plastic surgeon Christopher T. Maloney Jr. stretched the skin on her chest with temporary implants, called expanders, then he slowly filled them over time. Eventually, he replaced them with silicon implants.
After her first reconstruction procedure, she found herself in unbearable pain, stuck on the couch and unable to move. She couldn't reach her cell phone or her pain medication.
Her 18-year-old daughter, Shira Wolf, happened to stop by and came to her rescue.
"I know it was normal for her to be in pain, but it's hard to watch her go through it," Wolf said.
She's been at her mother's side, knowing that she may be faced with this decision some day. There's a 50 percent chance that she has the genetic mutation.
Rather than rush off to get tested, Wolf said, she wants to wait until she's in her 30s and has started a family.
"It's really scary thinking at a young age that you can get something and die and have no control over it. I don't want to live my life in fear," said Wolf, who is a senior at Catalina Foothills High School and the president of the National Honor Society.
Taking a cautious approach, she'll begin monitoring her breast health with mammograms and MRIs when she's 25 — 15 years sooner than what is recommended for the average woman.
Sometimes the teen is sure she doesn't want a preventive mastectomy. "I just can't imagine putting myself through that kind of pain."
Other times, she thinks she'll do it if that is her best option.
"I'm happy that she did it. . . ," she says of her mom. "I'm thankful my mother will be with me."
Wolf is young, and she's hoping the future will bring medical advances that make her choice easier.
For now, her mother is part of a growing trend. The clinic doctors say that as more women are identified with the BRCA-1 and BRCA-2 genetic mutations, which were discovered in the mid-'90s, they will follow in Diamond-Rivera's footsteps.
The last stages of Diamond- Rivera's breast reconstruction involved creating a new nipple by carving a star-shape in her breast and folding flaps of skin to form the nipple. To cover the scarring and make the nipple appear more real, the plastic surgeon will later tattoo an areola around the outside.
"It was so easy. I was so worried. I think it will really look like a real breast when it's healed and done," said Diamond-Rivera.
Her insurance has covered almost everything so far. Most insurance companies cover about 80 percent of the genetic testing, said genetic counselor Jessica Ray. The cost of the test without insurance is $2,975.
Many women are concerned that if they are identified as carriers of genetic mutations, their insurance companies will drop them, Ray said, but federal and Arizona state laws prohibit genetic discrimination.
Catherine Green, a 36-year-old who moved to Tucson about five years ago from New York, chose not to test herself for the BRCA genetic mutations when she first heard the tests were available. That was almost 10 years ago and before the laws against genetic discrimination were in place. She's been monitoring her breast health with mammograms and MRIs.
In November 2003, she was tested at the Arizona Cancer Center and learned that she carried the BRCA-2 genetic mutation. It is associated with an 87 percent risk for breast cancer and up to a 20 percent risk for ovarian cancer.
She continued to monitor her breast health closely.
"I wanted to stay intact as long as possible," said Green, who's an avid hiker and mountain biker.
It wasn't until doctors found precancerous cells in a recent biopsy that she started considering a mastectomy.
"That was the smoking gun I was waiting for," said Green.
After a second breast biopsy to confirm that she has precancerous cells, she will plan a mastectomy within the year.
"My whole goal was to catch it early, and I feel I have succeeded in it," Green said.
Green's not ready to remove her ovaries. She and her fiance are planning a wedding for this summer.
She doesn't want to endure premature menopause and doesn't want to close the door to having kids some day.
When school's out, Diamond-Rivera will have her hysterectomy — she decided to have both her ovaries and uterus removed — and take the summer off to rest. In the meantime, she's getting accustomed to her new breasts and has been bra shopping with her daughter, trying to find the best fit for her body.
Diamond-Rivera, Wolf and Green are joining as many as 11,000 participants in today's Race for the Cure.
"So many people have breast cancer. One day, it will probably be me. If not, it will be one of my friends," Wolf said.
"All we can do is make people aware."
● The doctors at the High-Risk Breast and Ovarian Cancer Clinic want to provide options and resources for patients and physicians.
● Preventive surgery is just one of many options for patients at the clinic. Doctors counsel patients through a variety of options, which include closely monitoring breast health with MRIs and ultrasounds, making lifestyle changes like exercising and maintaining an ideal body weight, or taking Tamoxifen, an anti-estrogen drug that reduces the chance of breast cancer in high-risk patients.
● To contact the clinic, call 326-5290 8 a.m.-5 p.m. Monday-Friday. Clinic appointments are the second and fourth Friday of every month, from noon to 4 p.m. Staff members screen patients by phone to make sure they have a risk factor.