WASHINGTON — An unprecedented effort to reverse the effects of a racially biased medical test that blocked or delayed Black people from getting kidney transplants seems to be working.
Researchers reported Monday that thousands of Black transplant candidates have been given credit on the transplant waiting list for time they lost because of that misguided test, moving up their priority in an attempt at restorative justice.
That test used a race-based formula to calculate patients’ kidney function. It made Black patients’ kidneys appear healthier than they really were, delaying diagnosis of impending organ failure and referral for transplant.
After the U.S. transplant system ended use of the race-based test, it ordered hospitals to determine which Black patients on their transplant lists could have qualified for a new kidney sooner, by combing medical records for long-ago biased findings, and credit them with that time.
People are also reading…
Researchers at Beth Israel Deaconess Medical Center, Brigham and Women’s Hospital and Boston Medical Center analyzed a database of all kidney transplants between January 2022 and June 2025, comparing transplant rates before and after the January 2023 policy change.

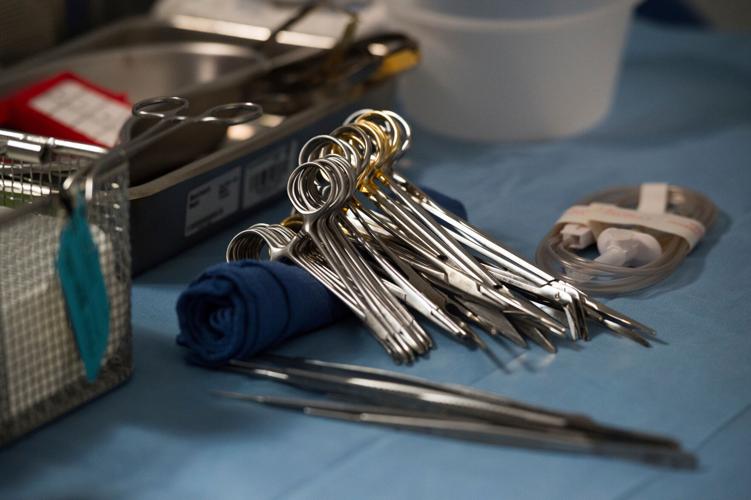
Surgical instruments and supplies lay on a table during a kidney transplant surgery at MedStar Georgetown University Hospital on June 28, 2016, in Washington D.C.
Among the more than 21,000 Black transplant candidates given waiting time modifications, the median gain was 1.7 years, the team reported in JAMA Internal Medicine. That's meaningful time as the wait for a kidney transplant averages three to five years but can be far longer in some parts of the country.
Black patients’ transplant rate increased right after the policy change, by 5.3 transplants per 1,000 listings, before leveling off. Overall the kidney transplant rate increased during the study period and the the transplant rate for non-Black patients didn't change significantly under the new policy, remaining highest for white patients., the researchers reported.
The findings “suggest that improving transplant care for Black individuals did not harm individuals of other races,” Dr. L. Ebony Boulware of Wake Forest University School of Medicine, who wasn’t involved in the study, wrote in an accompanying commentary that urges similar efforts to mitigate harm from other erroneously race-based medical tests.
The policy “hopefully helps move the needle toward equity,” Dr. Rohan Khazanchi of Brigham and Women’s Hospital and Boston Medical Center, who led the study, said in an interview.

A sign hangs from the Beth Israel Deaconess Medical Center on Aug. 18, 2022, in Boston.
Getting a wait-time credit didn't translate into immediate transplants — 7,484 of them received a new kidney during the study period.
The biased kidney test was based on a measurement of how quickly a waste compound called creatinine gets filtered from blood. In 1999, an equation used to calculate that rate was modified to adjust Black people’s results compared to everyone else’s, based on some studies with small numbers of Black patients and a long-ago false theory about differences in creatinine levels.
That test exacerbated other disparities that already make Black Americans more at risk of needing a new kidney but less likely to get one. They are over three times more likely than white people to experience kidney failure and make up about 30% of the kidney transplant list.
Khazanchi was surprised to find that less than 1 of 3 Black transplant candidates received wait-time modifications.
That might be because some weren’t diagnosed with kidney disease until their organs had failed, an emergency that doctors call “crashing onto dialysis.” But Khazanchi said another possibility is that some transplant centers had more resources than others to do the digging into old medical records – lab tests performed not only years earlier but possibly in different health systems in different parts of the country – to find everyone who qualified.
While the ordered lookback to change wait times happened in 2023, Black patients more recently added to the transplant list should ask if they also may be eligible, he advised.